CLICK TO SHOP OUR BLACK FRIDAY SALE!
*Excludes BioNude and subscriptions
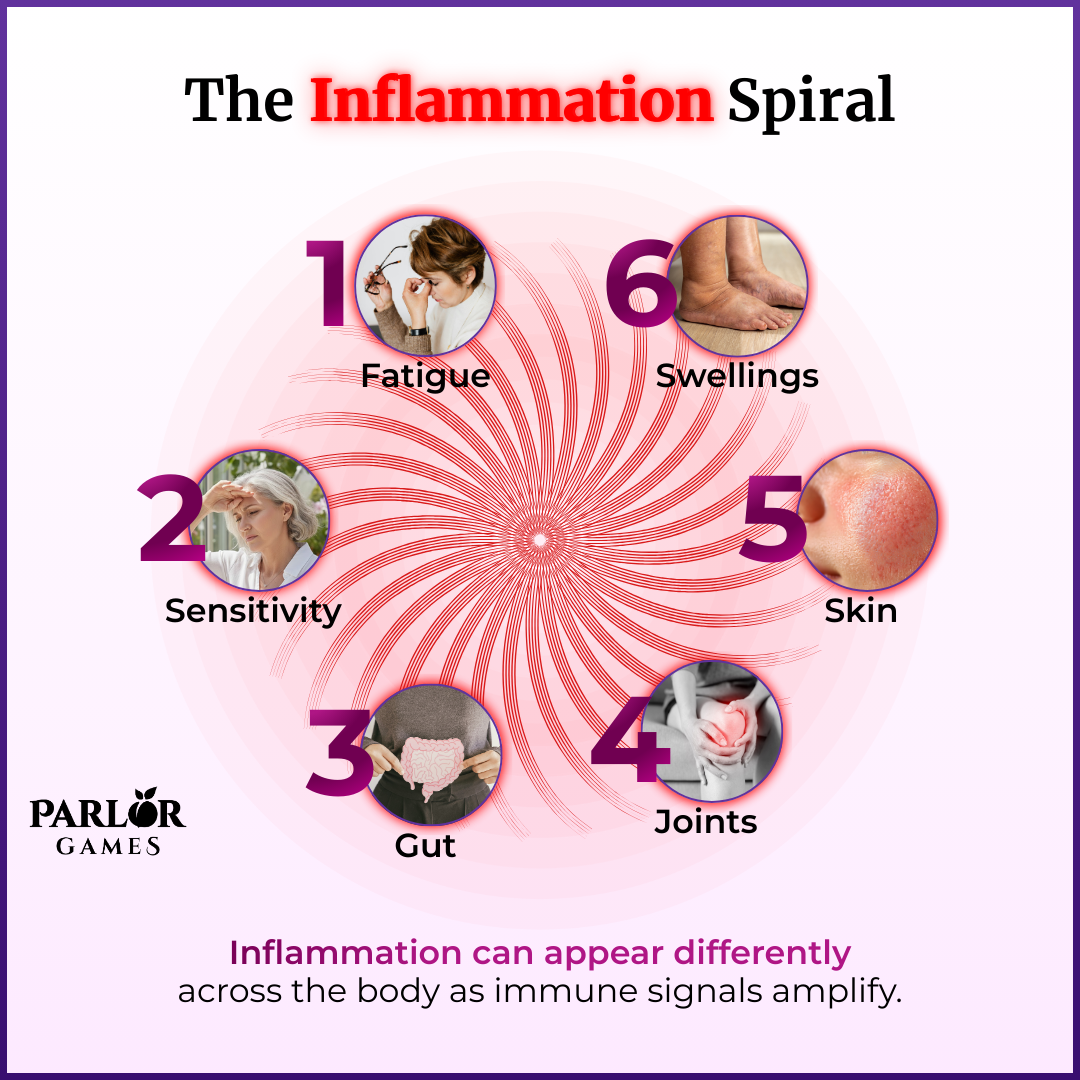
A familiar pattern starts to appear...
What many women report as they enter perimenopause and menopause is a rise in inflammation, immune reactivity, or autoimmune-like symptoms - often without a clear medical explanation. However, there actually is a well researched link between hormonal shifts, immune regulation, and inflammatory response in women.
Women experience autoimmune issues at dramatically higher rates than men - about 80% of autoimmune diagnoses occur in women.
Why might this be? While autoimmunity is a complex situation, we do know that hormones can be a contributing factor. Estrogen, progesterone, DHEA, testosterone, and the stress hormone cortisol all influence how immune cells behave.
Evolutionarily, this was a strength; women needed robust immunity to survive infections during pregnancy, breastfeeding, and communal caregiving. However, the trade-off is that women also have more immune system volatility, especially when hormones shift. During the reproductive years, estrogen and progesterone help keep the immune system balanced. In perimenopause and menopause when hormone levels are first variable, and later, low, those regulators can go a little haywire.
This is when many women first notice:
The immune system is responsive and hormones play a role in immune regulation.
Inflammation is meant to be a controlled, temporary response, but when hormones begin to fluctuate or decline, that control system wobbles.
In perimenopause and menopause, women commonly experience:
So much of autoimmunity is a slow steady wave.with gentle curves and low amplification. As hormones begin to fluctuate - often combined with highly stressful stages of a woman's life, the wave amplification becomes more pronounced.
Take exercise for example. A 30 year old woman does a 20 mile hike; she feels fine the next day because her immune system responded to the increased demand on a range of body systems and handled it. A 50 year old woman does a 20 mile hike and it can take three days for the inflammatory demand to resolve; she may have swollen ankles, or aching knees, she may be more tired and feel a loss in stamina. If she has an underlying autoimmune condition, it could take even longer to recover, for her, the amplitude of the inflammatory response wave is steeper.
Estrogen increases immune activity, stimulating antibody production and inflammatory signaling. Too much can overactivate immune response, too little can reduce natural modulation of the immune response.
Progesterone calms immune activity, reduces excessive inflammation, and protects barrier tissues (skin, gut lining, bladder, and vaginal tissue). Low progesterone, which typically starts in perimenopause (or even earlier) leaves the immune system with fewer sources for regulation.
Dehydroepiandrosterone (DHEA): The Wellness Hormone
DHEA improves cellular immunity, provides antioxidant effects, improves blood flow (which reduces increase in clearing toxicants from the body), balances elevated cortisol and, of course, is the precursor hormone for testosterone, estradiol, and estriol. DHEA levels decline steadily from age 30 onwards.
Cortisol is an anti-inflammatory hormone when stable. When sleep changes, stress rises, or cortisol becomes dysregulated, inflammation becomes harder to control.
For women who already have autoimmune condition, the perimenopausal/menopausal transition can amplify all the associated issues.
So, why the amplifications? At the root of this is the immune systems’ already established tendency toward overactivity. When progesterone drops, estrogen fluctuates, and cortisol becomes too high or too low, the immune system receives mixed signals, often increasing sensitivity and inflammation still further.
Common experiences women report include:
This doesn’t mean hormones cause autoimmune disease - however, hormonal change can amplify the underlying immune dysregulation that some women already have.
Understanding what is hormonal vs. autoimmune vs. stress-driven often becomes clearer with testing, especially saliva hormone testing, which evaluates the cortisol curve alongside estrogen, DHEA, and progesterone levels.
Around 70% of the immune system lives in the gut, which means any shift in gut balance can trigger inflammatory or autoimmune-like symptoms, and hormones profoundly influence the gut environment.
When these hormones decline:
This creates a feedback loop where the immune system stays activated, even without an infection.
Estrogen supports beneficial gut bacteria. When estrogen drops, the microbiome can be affected including a decline in beneficial bacteria and an increase in harmful bacteria. This shift can contribute to autoimmune activity or feelings of systemic inflammation.
Many women notice vaginal changes (often called vaginal atrophy or attributed to Genitourinary Syndrome of Menopause) in perimenopause and menopause:
Why? Because the vaginal microbiome also depends on estrogen. Low estrogen reduces glycogen in vaginal tissues, which reduces lactobacillus (the bacteria that keep vaginal pH healthy and protective).
This can create:
When the gut becomes inflamed, the vaginal ecosystem often changes as well, which is why some women experience both gastrointestinal (GI) symptoms and vaginal discomfort during the same hormonal window.
Any autoimmune condition must be discussed with a specialist practitioner. Understanding the impact of changing hormone levels in inflammation helps you explore changes in your body through that lens. Knowing your individual hormone levels can provide insight into how you, just you, no one else, are experiencing the hormone changes associated with perimenopause and menopause. Hormone supplementation isn’t for everyone, yet knowing low hormones can exacerbate inflammation gives you key information when you are looking for lasting solutions.
This gives insight into:
Many women find a lot of relief in seeing whether symptoms align with:
Progesterone is naturally calming to the immune system. It reduces inflammatory signaling and supports barrier tissues, including the gut and vaginal mucosa.
Women who explore progesterone support (such as Vibrant Third Progesterone, used under provider guidance) often describe better sleep, more emotional steadiness, less inflammatory sensitivity, and more resilience to stress.
"I have been so pleased so far with the difference Vibrant Third has made - it has seemed to really help my brain fog, and I think its also helping with some inflammation issues I have been struggling with. I am working on my application schedule to find my 'happy place' - I like it, and I am about 6 weeks in!" - ✅Phyllis
"...arthritis aches and pains have dropped from daily misery inducing to occasional flares... My energy levels are up! I don't need to take a nap after a 3 mile walk. I can do a full day at school and swim practice and still have the desire to spend a night out with my husband. I am SO glad to have found this company and these products!" - ✅SueMo1017
Autoimmunity and inflammation in midlife don’t develop out of nowhere; these concerns become more noticeable when the hormonal regulators that keep the immune system balanced begin to shift.
Understanding your hormonal environment (especially progesterone, DHEA, and cortisol) can help you make more informed choices about testing, lifestyle adjustments, and in discussions with your healthcare provider. Your immune system isn’t betraying you. It’s responding to a new hormonal landscape - and you are absolutely capable of understanding and navigating it.
References

Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Disclaimer: The information provided above is intended for educational and informational purposes only. Statements made have not been evaluated by the FDA nor are they intended to treat or diagnose. Any health concerns should be discussed and evaluated by your primary health care provider.
Parlor Games, LLC ● kate@parlor-games.com ● 5304 River Rd N Ste B ● Keizer OR 97303
Disclaimer: The information provided above is intended for educational and informational purposes only. Statements made have not been evaluated by the FDA nor are they intended to treat or diagnose. Any health concerns should be discussed and evaluated by your primary health care provider.
28 Day Challenge Subscription Details

We ship you a 28 day supply of Silky Peach Cream for only $29 (more than 25% off our normal price) when you sign up for Subscribe & Save.
Follow the directions we include in the package and apply Silky Peach cream on your tender bits for 28 days.

Decision Day:
5 days before your subscription rebills, we’ll send you an email reminder with a link. If you decide Silky Peach is nice but not your thing… you can click that link and cancel your subscription without even talking to anyone. No hassle — no questions asked.
If you are like 72% of our Silky Peach customers, you’ll love it and can't imagine life without it. In that case, do nothing, and we’ll welcome you to the Parlor Games family and ship Silky Peach Cream to your door step every month for the same discounted price of $29 — locked in for as long as you remain a subscriber.

Important note about our easy-breezy subscriptions:
We know that some companies make it hard to cancel a subscription — that’s not us. Our mission is to save the world — one vagina at a time! If you decide you don’t need Estriol as an ongoing solution for dryness, incontinence, UTIs and keeping sex fun and comfortable again, we understand. Five days before we ship your next order, you'll receive an email with a link to cancel right there in the message.
No hunting, no searching, we got you. Respect is where it’s at.
FYI – Estriol is beneficial for skin integrity and mucous membranes. It’s great for vaginal atrophy and also amazing for use on the face and neck. Applying a small amount — about 1 pump — can help build the collagen and plump up the cells to reduce wrinkles. Who knew!!
OUR HAPPINESS GUARANTEE
We want you to feel safe and confident trying any of our products. That's why we promise 100% money-back guarantee on the purchase price of the first bottle of any of our products. Balancing hormones DOES take some time, so please try it for 28 days. If after 28 days you are unhappy, or the product just hasn't worked for you, simply contact us and we'll process a refund of your full purchase price upon receipt. Sorry, shipping fees are not refundable.