CLICK TO SHOP OUR BLACK FRIDAY SALE!
*Excludes BioNude and subscriptions

Pelvic floor therapy is a specialized form of physical therapy focused on the muscles, connective tissues, and nerves that support the bladder, bowel, uterus, and vagina. These muscles are responsible for continence, sexual function, core stability, and pelvic organ support. When they are not functioning properly, the effects can show up in ways that are often dismissed as “normal,” especially for women.
Pelvic floor therapy is a specialized form of physical therapy focused on the muscles, connective tissues, and nerves that support the bladder, bowel, uterus, and vagina. These muscles are responsible for continence/incontinence, sexual function, core stability, and pelvic organ support. When they are not functioning properly, the effects can show up in ways that are often dismissed as “normal aging”... especially for women.
We hear from women who note that they have to bend over completely to empty their bladders, or women who are constantly doing kegels and yet cannot kick incontinence, and from women who live with sexual pain for years that they cannot understand.
Pelvic floor therapy aims to restore proper muscle coordination, strength, relaxation, and tissue health. It is not just about strengthening. In fact, many pelvic floor issues stem from muscles that are overactive, tense, or poorly coordinated rather than weak.
Pelvic floor therapy can be used in the context of pain, leakage, prolapse symptoms, sexual dysfunction, and postural or core instability. It is relevant across the lifespan but becomes especially important during perimenopause and menopause, when hormonal changes can alter tissue integrity and muscle function.
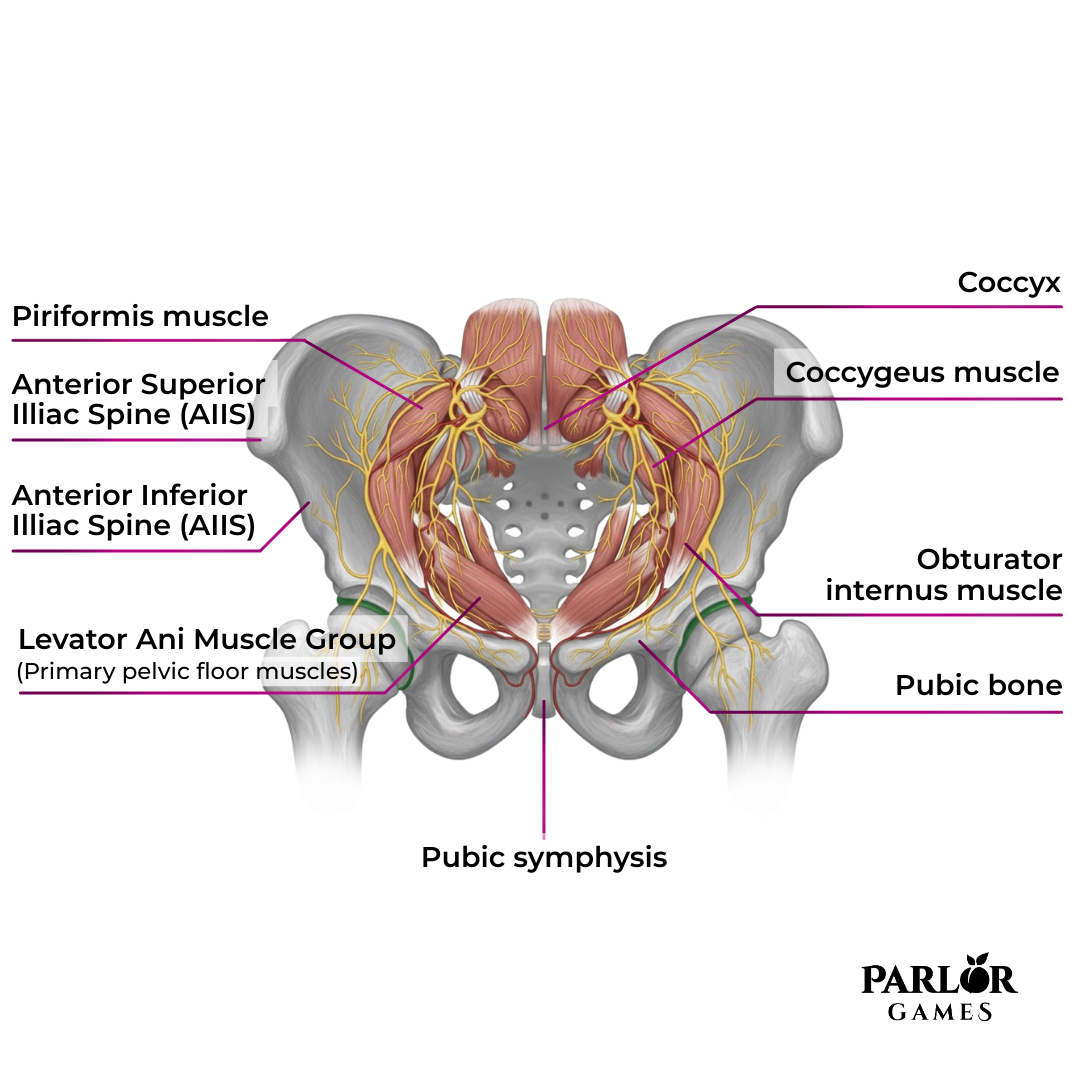
The pelvic floor is not a single muscle. It is a layered, bowl-shaped complex of muscles, fascia, and connective tissue that spans the bottom of the pelvis. These muscles attach to the pubic bone, tailbone, and sit bones, forming a supportive ‘sling’ for the pelvic organs.
Key functions of the pelvic floor include:
• Supporting the bladder, uterus, and rectum
• Maintaining urinary and bowel continence
• Coordinating with the diaphragm and deep abdominal muscles for core stability
• Playing a key role in sexual sensation and orgasm
• Responding reflexively to pressure changes such as coughing, lifting, or laughing
The pelvic floor works as part of a larger system that includes the diaphragm, deep core muscles, and hip stabilizers. Dysfunction in any part of the system can affect pelvic floor performance overall.
Healthy pelvic floor muscles both contract and fully relax. Chronic tension, guarding, or poor relaxation can be just as problematic as weakness and often leads to pain, urinary urgency, and sexual discomfort.
When most people hear “pelvic floor,” they think Kegels… kegels, kegels, and more kegels. Tighten, squeeze, repeat. And while Kegels have their place, they are often over-prescribed and, without guidance in pelvic floor therapy, frequently done incorrectly.
Remember, pelvic floor dysfunction is not always about weakness.
In many women, especially during perimenopause and menopause, the pelvic floor is already overactive, tense, or holding. This can happen due to pain, tissue irritation, hormonal changes, chronic stress, or organ prolapse. In this situation, adding more squeezing through Kegels can worsen symptoms.
Kegels focus on strengthening the pelvic floor muscles by repeated contraction. This can be helpful for true muscle weakness, such as certain cases of stress urinary incontinence. But kegels do not address coordination, relaxation, breathing patterns, tissue health, or nerve sensitivity.
Pelvic floor therapy looks at the entire system. This includes how the muscles contract, how fully they relax, how they respond to pressure, and how they interact with the diaphragm, hips, and deep core.
In a nutshell, kegels are one tool - pelvic floor therapy is the toolbox. 🧰
Pelvic floor dysfunction occurs when the muscles of the pelvic floor are unable to coordinate properly. This can mean they are too weak, too tight, slow to respond, or unable to relax when they should.
Common symptoms include:
• Urinary leakage or urgency
• Difficulty fully emptying the bladder or bowels (i.e., having to lean/move to fully empty)
• Pelvic pain or pressure
• Pain with penetration or tampon use
• Low back, hip, or tailbone pain
• Sensation of heaviness or bulging
Pelvic floor dysfunction can occur as a combination of many factors: pregnancy, childbirth, chronic stress, repetitive high-impact exercise, trauma, surgery, and aging can all play a role. Menopause adds another layer by altering tissue quality and neuromuscular signaling.
During menopause, declining estrogen affects blood flow, collagen density, nerve sensitivity, and tissue elasticity throughout the pelvic region. This can make muscles less responsive, tissues more fragile, and recovery from strain slower.
Women may experience new pelvic symptoms even without a history of childbirth or injury. Pelvic floor therapy addresses both muscular coordination and tissue support, making it a critical but underutilized intervention during this stage of life.
These are not generic “just do more Kegels” tips. These are strategies recommended by specialist pelvic floor therapists to support pelvic floor function, especially as hormone levels diminish.
Many women have never consciously relaxed their pelvic floor muscles. Chronic tension can contribute to pain, urinary urgency, incomplete emptying, and discomfort with sex.
Practicing slow diaphragmatic breathing helps the pelvic floor move naturally with the breath. As you inhale, the pelvic floor should gently lengthen and descend. As you exhale, it recoils and lifts. This coordination is foundational.
If you cannot fully relax the pelvic floor, strengthening exercises will not work properly.
The pelvic floor works in partnership with the diaphragm and deep abdominal muscles. Holding your breath during exercise, lifting, or daily tasks increases downward pressure on the pelvic floor.
Exhaling during effort helps reduce strain and supports better muscle coordination. This is especially important during menopause, when connective tissue support is reduced.
Pelvic floor muscles do not function well when surrounding tissues are dry, thin, irritated, or painful. Estrogen loss during menopause affects vulvar, vaginal, and urethral tissues, which can drive muscle guarding and altered movement patterns.
Supporting tissue hydration, elasticity, and comfort allows pelvic floor muscles to relax and engage appropriately. This is why hormonal support and pelvic floor therapy often work well together.
Constantly pulling in your stomach or clenching your glutes creates excess tension in the pelvic floor. This habitual bracing is common in women and often worsens during stressful life stages.
Your core is meant to respond dynamically, not stay locked down. Learning to let go of unnecessary tension improves pelvic floor mobility and reduces symptoms over time.
Pelvic floor dysfunction cannot be accurately self-diagnosed. A trained pelvic floor physical therapist can assess muscle tone, coordination, strength, relaxation, and tissue response.
This assessment determines whether you actually need strengthening, relaxation, coordination work, or a combination. It also helps prevent doing the wrong exercises for your specific pattern.
Recommended resource: Dr. Sara Reardon's book Floored is the pelvic floor resource we wish every woman had on her nightstand, and her new app The V-Hive makes personalized pelvic floor support accessible wherever you are. We're big fans. Find her at thevagwhisperer.com.
In menopause, declining estrogen can lead to thinner, more sensitive tissues that are more prone to irritation and micro-injury. This can directly affect pelvic floor function. Fragile tissues may increase muscle tension, pain, and altered muscle firing patterns. In these cases, restoring tissue comfort and flexibility is just as important as muscle training.
Estriol is the gentlest form of estrogen and can play a crucial role in maintaining the health of vulvar, vaginal, and lower urinary tract tissues. While estradiol is often prescribed for systemic delivery of estrogen, estriol is particularly important for tissue integrity, hydration, and elasticity in the pelvic region.
Estriol supports:
• Thickness and resilience of vaginal and vulvar tissues
• Healthy mucous membranes
• Acidic vaginal pH that protects against infection
• Collagen reserves needed for tissue repair
Pelvic floor therapy is optimized when tissues are capable of responding to therapy. In menopausal women, addressing estriol deficiency, with Silky Peach Estriol Cream, can improve tissue quality, reduce discomfort, and allow pelvic floor muscles to relax and engage more effectively.

Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Disclaimer: The information provided above is intended for educational and informational purposes only. Statements made have not been evaluated by the FDA nor are they intended to treat or diagnose. Any health concerns should be discussed and evaluated by your primary health care provider.
Parlor Games, LLC ● kate@parlor-games.com ● 5304 River Rd N Ste B ● Keizer OR 97303
Disclaimer: The information provided above is intended for educational and informational purposes only. Statements made have not been evaluated by the FDA nor are they intended to treat or diagnose. Any health concerns should be discussed and evaluated by your primary health care provider.
28 Day Challenge Subscription Details

We ship you a 28 day supply of Silky Peach Cream for only $29 (more than 25% off our normal price) when you sign up for Subscribe & Save.
Follow the directions we include in the package and apply Silky Peach cream on your tender bits for 28 days.

Decision Day:
5 days before your subscription rebills, we’ll send you an email reminder with a link. If you decide Silky Peach is nice but not your thing… you can click that link and cancel your subscription without even talking to anyone. No hassle — no questions asked.
If you are like 72% of our Silky Peach customers, you’ll love it and can't imagine life without it. In that case, do nothing, and we’ll welcome you to the Parlor Games family and ship Silky Peach Cream to your door step every month for the same discounted price of $29 — locked in for as long as you remain a subscriber.

Important note about our easy-breezy subscriptions:
We know that some companies make it hard to cancel a subscription — that’s not us. Our mission is to save the world — one vagina at a time! If you decide you don’t need Estriol as an ongoing solution for dryness, incontinence, UTIs and keeping sex fun and comfortable again, we understand. Five days before we ship your next order, you'll receive an email with a link to cancel right there in the message.
No hunting, no searching, we got you. Respect is where it’s at.
FYI – Estriol is beneficial for skin integrity and mucous membranes. It’s great for vaginal atrophy and also amazing for use on the face and neck. Applying a small amount — about 1 pump — can help build the collagen and plump up the cells to reduce wrinkles. Who knew!!
OUR HAPPINESS GUARANTEE
We want you to feel safe and confident trying any of our products. That's why we promise 100% money-back guarantee on the purchase price of the first bottle of any of our products. Balancing hormones DOES take some time, so please try it for 28 days. If after 28 days you are unhappy, or the product just hasn't worked for you, simply contact us and we'll process a refund of your full purchase price upon receipt. Sorry, shipping fees are not refundable.