CLICK TO SHOP OUR BLACK FRIDAY SALE!
*Excludes BioNude and subscriptions
We are all familiar with the unpleasant ‘someone has threaded wire into my urethra’ feeling that signals the dawning of a UTI.
What starts as a small discomfort quickly turns to full blown burning and stinging every time we sit down to pee. We are then stuck in a catch-22; drink less means pee less, but worse for UTI, drink more is better for UTI, but then pee more. 😭 Right as we plan to get on a plane for several hours...!
We have some great blogs on ways to keep the vagina, bladder and entire genitourinary complex UTI free (Hello, D-Mannose…), but something that is equally important is understanding a few key things:
1. Why do UTI’s often become more frequent as we age?
2. Why aren’t antibiotics working, or, why do they work only for a UTI to return a week later?!
3. How does UTI presentation change with age (yes, sometimes we don’t FEEL a UTI!)
4. What are the dangers of repeat (or untreated) UTI’s?
So, let’s take a look…
There are some basics to UTI hygiene that many women already know - things like avoiding soap in the urethra, avoiding using pads that can transfer bacteria, peeing after sex, and changing out of sweaty lycra. Plus, there are the well known lifestyle factors - things like drinking enough water and avoiding sugar, that can play a role in UTI frequency and severity.
But let’s face it, getting a UTI once a month isn’t adding up even if you did hang out in sweaty lycra and skip water at lunch.
There is a strong link between estrogen levels and UTI frequency, especially as women go through menopause and beyond. Estrogen is critical for urethral, vulva, and vaginal health and the drop in estrogen after menopause often means an increase in UTI’s. Estrogen - and in particular estriol - the gentlest form of estrogen can really help.
How? Well, let’s take a look at some of the key ways:
Skin cell health: The decline in estrogen means it is important for keeping the outer layer of cells healthy and - perhaps most importantly - encouraging healthy cell turnover.
Collagen reserves: collagen (as we may all know from constant advertising bombardment…) keeps wrinkles at bay - but it also helps repair tissue damage. As we age, the skin of the urinary tract (and vulva and vagina) loses collagen and starts to thin. Thinning skin can result in small micro tears. Collagen helps with repair and wrinkle fighting - something that is needed to prevent bacteria transfer. And, estrogen is important for collagen formation.
pH Balance: the Vaginal Microbiome is acidic, which helps kill off bacteria that should not be there - but without estrogen, the pH can rise, creating an environment where bacteria can flourish. More vaginal bacteria can increase the chance of spreading to the urethra.
Mucous membranes: One of estrogen’s super important functions is mucous membrane health. When mucous membranes ‘get thinner’ we feel this as a drying of the tissue. This has a big ripple effect - we itch more (and/or apply things to mitigate itch), leading to weaker skin, more damage, and more ways for bacteria to thrive - and move around - and potentially enter the urethra!
So, it’s not one simple problem, but more the overall decline in estrogen that creates an environment where bacteria can get a stronger foothold and have an easier time spreading from anus, perineum, and vagina, into the urethra.
But, if a UTI is just bacteria, why doesn’t a good strong dose of antibiotics do the job?
Well, there are a few reasons for this one too…
Issue | What It Means | Why It Matters |
Different bacteria cause UTIs | Most are E. coli, but others (Klebsiella, Proteus, Enterococcus) require different meds. | The antibiotic that works for one organism may do nothing for another. |
Antibiotic resistance | Some bacteria have adapted and no longer respond to common antibiotics. | Symptoms persist or return quickly because the drug couldn’t kill the bacteria. |
Recurrent infections may involve new organisms | Not every “repeat UTI” is the same bacteria coming back. | Each infection may require a different targeted treatment. |
Incorrect or incomplete treatment | Short or mismatched courses allow bacteria to linger. | Leads to chronic inflammation, recurring symptoms, and more antibiotic use. |
Repeated courses of antibiotics can disrupt the vaginal and gut microbiomes, eliminating not only harmful bacteria but also the good bacteria that help maintain pH, immune function, and tissue integrity.
This disruption makes women more prone to yeast infections, digestive problems, and (ironically) future UTIs. Heavy antibiotic exposure also increases the chance of antibiotic resistance, meaning the usual medications may stop working as well. This doesn’t mean antibiotics should be avoided when they’re needed; it simply means that prevention, tissue support (like estriol for mucosal health), and targeted treatment strategies matter!
No really.
As many of us become caregivers to elderly parents (or already are), it is important to understand the seriousness of UTI’s; what can be a nuisance in our younger years can be much more dangerous to older women - and so UTI’s often get missed.
In fact, studies have shown that not only are UTI’s one of the most frequently diagnosed infections in older adults (between 15-30%), around 6.25% of infection-related deaths in elderly patients are attributed to UTI’s.
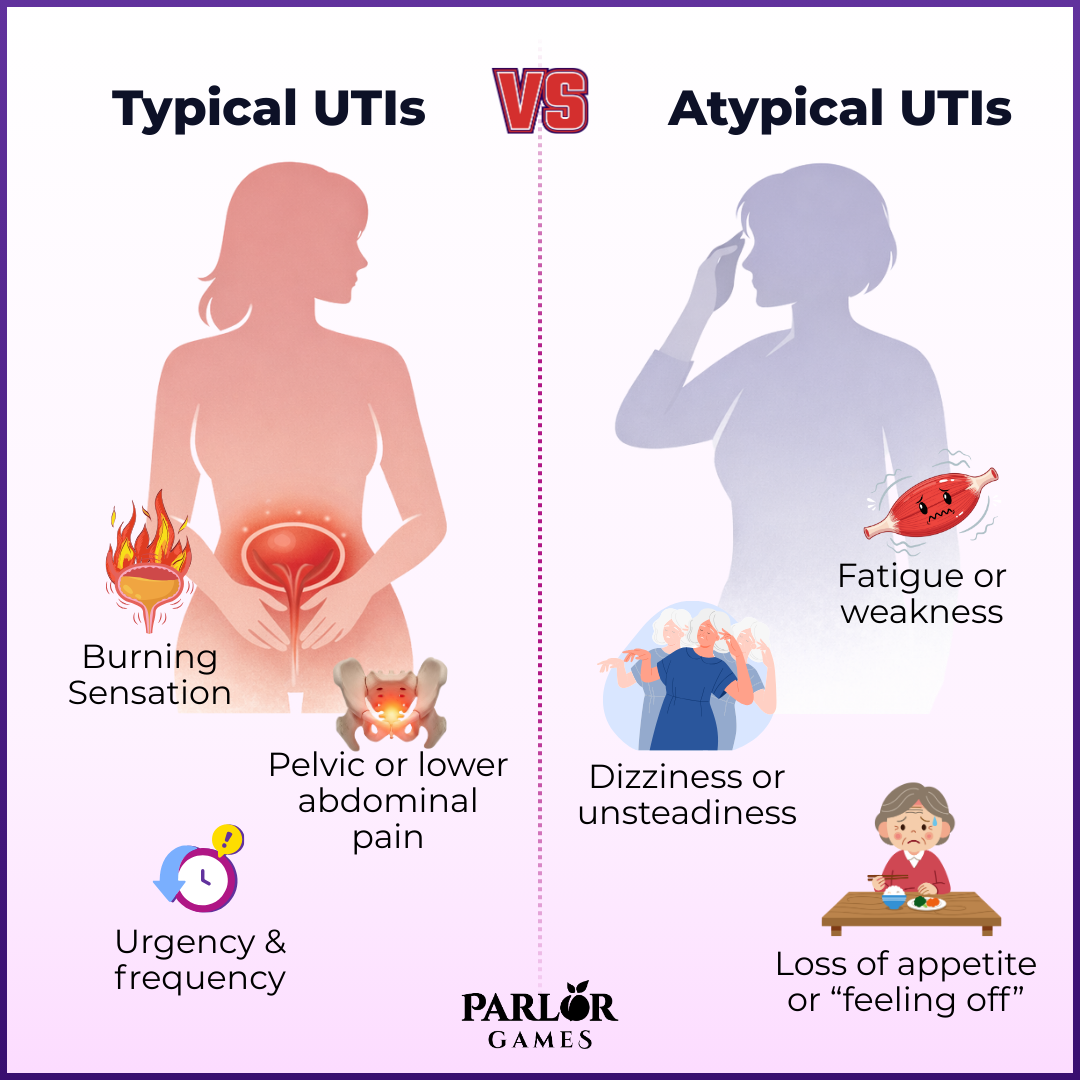
Let’s compare:
🔥 Burning with urination (dysuria)
🚽 Urgency and frequency
🌫️ Cloudy or strong-smelling urine
⚡ Lower abdominal or pelvic pain
🩸 Occasionally blood in urine
❗Symptoms appear quickly and are easy to identify
🧠 Mental status stays normal
🦠 Usually localized infection without systemic symptoms
🧩 Fewer urinary symptoms - often no burning
💤 Generalized fatigue or “feeling off”
🤒 Low-grade fever or no fever at all
🧠 Confusion, delirium, agitation, or sudden behavioral change
🥴 Dizziness, falls, or unsteadiness
🍽️ Loss of appetite
⚕️ Worsening of existing conditions (incontinence, dementia, frailty)
🩺 Symptoms may be vague, slow to appear, or misattributed to “age”
🚑 Higher risk of rapid progression to serious infection (e.g., kidney infection or sepsis)
As you can see - for younger women, or UTI’s with more common symptoms stay localized to the vaginal-urethral complex, with some women complaining of pelvic or abdominal pain. In comparison, for older women , there are often more cognitive issues that caregivers may not associate with UTI’s.
An untreated UTI doesn’t always stay “just a bladder infection.” In many women (especially in midlife and beyond) the bacteria can travel upward from the bladder into the kidneys. Kidney infections (pyelonephritis) can lead to high fever, lower back pain, and sometimes hospitalization. If the infection continues to spread, it can enter the bloodstream, causing urosepsis, which is serious but preventable with timely treatment.
Even when complications don’t escalate that far, untreated infections can still cause ongoing inflammation, bladder irritation, and worsening urgency or frequency that disrupt daily life. While not everyone will be affected this way, it’s vital to solve a UTI to reduce the risk of it getting complicated.
Someone with repeat UTI’s does need to have a longer conversation with their doctor about what are the options for a lasting solution. There is however, some cool science about estrogen that is worth knowing.
From the 50 year old with recurrent UTI’s to the 80 year old - estriol offers the ability to replenish estriol and supply the tissues with the necessary building blocks to manage long-term UTI prevention.
Silky Peach cream offers topical estriol that can be applied directly to the skin of the vulva, helping replenish estriol and rejuvenate the tender tissues and maintain the overall health and integrity of the entire genitourinary complex!
Watch more here:

Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Disclaimer: The information provided above is intended for educational and informational purposes only. Statements made have not been evaluated by the FDA nor are they intended to treat or diagnose. Any health concerns should be discussed and evaluated by your primary health care provider.
Parlor Games, LLC ● kate@parlor-games.com ● 5304 River Rd N Ste B ● Keizer OR 97303
Disclaimer: The information provided above is intended for educational and informational purposes only. Statements made have not been evaluated by the FDA nor are they intended to treat or diagnose. Any health concerns should be discussed and evaluated by your primary health care provider.
28 Day Challenge Subscription Details

We ship you a 28 day supply of Silky Peach Cream for only $29 (more than 25% off our normal price) when you sign up for Subscribe & Save.
Follow the directions we include in the package and apply Silky Peach cream on your tender bits for 28 days.

Decision Day:
5 days before your subscription rebills, we’ll send you an email reminder with a link. If you decide Silky Peach is nice but not your thing… you can click that link and cancel your subscription without even talking to anyone. No hassle — no questions asked.
If you are like 72% of our Silky Peach customers, you’ll love it and can't imagine life without it. In that case, do nothing, and we’ll welcome you to the Parlor Games family and ship Silky Peach Cream to your door step every month for the same discounted price of $29 — locked in for as long as you remain a subscriber.

Important note about our easy-breezy subscriptions:
We know that some companies make it hard to cancel a subscription — that’s not us. Our mission is to save the world — one vagina at a time! If you decide you don’t need Estriol as an ongoing solution for dryness, incontinence, UTIs and keeping sex fun and comfortable again, we understand. Five days before we ship your next order, you'll receive an email with a link to cancel right there in the message.
No hunting, no searching, we got you. Respect is where it’s at.
FYI – Estriol is beneficial for skin integrity and mucous membranes. It’s great for vaginal atrophy and also amazing for use on the face and neck. Applying a small amount — about 1 pump — can help build the collagen and plump up the cells to reduce wrinkles. Who knew!!
OUR HAPPINESS GUARANTEE
We want you to feel safe and confident trying any of our products. That's why we promise 100% money-back guarantee on the purchase price of the first bottle of any of our products. Balancing hormones DOES take some time, so please try it for 28 days. If after 28 days you are unhappy, or the product just hasn't worked for you, simply contact us and we'll process a refund of your full purchase price upon receipt. Sorry, shipping fees are not refundable.